|
NIH-funded mouse study identifies therapeutic target
for clearing out toxic proteins damaged during
neurodegenerative disorders.
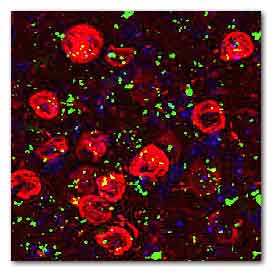
Proteasomes and Brain Cell Death: Using mouse brains, scientists studied the role of the proteasome system in neurodegenerative disorders.Karen Duff, Ph.D., Columbia University.
A study of mice shows how proteasomes, a cell’s
waste disposal system, may break down during
Alzheimer’s disease, creating a cycle in which
increased levels of damaged proteins become toxic,
clog proteasomes, and kill neurons. The study,
published in Nature Medicine and supported by the
National Institutes of Health, suggests that
enhancing proteasome activity with drugs during the
early stages of Alzheimer’s may prevent dementia and
reduce damage to the brain.
“This exciting research advances our understanding
of the role of the proteasomes in neurodegeneration
and provides a potential way to alleviate symptoms
of neurodegenerative disorders,” said Roderick
Corriveau, Ph.D., program director at the NIH’s
National Institute of Neurological Disorders and
Stroke (NINDS), which provided funding for the
study.
The proteasome is a hollow, cylindrical structure
which chews up defective proteins into smaller,
pieces that can be recycled into new proteins needed
by a cell.
To understand how neurodegenerative disorders affect
proteasomes, Natura Myeku, Ph.D., a postdoctoral
fellow working with Karen E. Duff, Ph.D., professor
of pathology and cell biology at Columbia
University, New York City, focused on tau, a
structural protein that accumulates into clumps
called tangles in the brain cells of patients with
Alzheimer’s disease and several other
neurodegenerative disorders known as tauopathies.
Using a genetically engineered mouse model of
tauopathy, as well as looking at cells in a dish,
the scientists discovered that as levels of abnormal
tau increased, the proteasome activity slowed down.
Treating the mice at the early stages of tauopathy
with the drug rolipram increased proteasome
activity, decreased tau accumulations and prevented
memory problems. They found that the drug worked
exclusively during the early stages degeneration,
which began around four months of age. It helped
four-month old tauopathy mice remember the location
of hidden swimming platforms as well as control
mice, and better than tauopathy mice that received
placebos. Treating mice at later stages of the
disease was not effective.
“These results show, for the first time, that you
can activate the proteasome in the brain using a
drug and effectively slow down the disease, or
prevent it from taking a hold,” said Dr. Duff,
senior author of the study.
Rolipram was initially developed as an
antidepressant but is not used clinically due to its
side effects.
It increases the levels of cyclic AMP, a compound
that triggers many reactions inside brain cells.
Rolipram works by blocking cyclic AMP
phosphodiesterase four (PDE4), an enzyme that
degrades cyclic AMP. The scientists found that
cyclic AMP levels are critical for controlling
proteasome activity. Treating brain slices from
tauopathy mice with rolipram, or a version of cyclic
AMP that PDE4 cannot degrade, reduced the
accumulation of tau and sped proteasome activity.
“We were hoping to show, using rolipram, that
increasing cyclic AMP is a pharmaceutical strategy
worth pursuing. The suggestion is not that rolipram
should immediately go into the clinic but that drugs
with mechanisms similar to rolipram should be
investigated further,” said Dr. Myeku.
Drs. Myeku and Duff plan to further investigate
proteasome activity and the impact of tau and other
disease-related proteins on this system for chewing
up and clearing out damaged proteins. In addition,
they want to search libraries of FDA-approved
compounds or new molecules for drugs that work in a
similar way to rolipram or activate proteasomes by
different pathways.
“The proteasome system we are studying also degrades
proteins associated with a number of other
neurodegenerative diseases such as Parkinson’s,
Huntington’s, frontotemporal degeneration and
amyotrophic lateral sclerosis. We may be able to
apply these findings to other disorders that
accumulate proteins,” said Dr. Duff.
For more information
Myeku N et al. “Tau-driven 26S proteasome impairment
and cognitive dysfunction can be prevented early in
disease by activating cAMP-PKA signaling,” Nature
Medicine, December 21, 2015.
Link...
National Institute of Neurological Disorders and
Stroke (NINDS)
Link...
MDN |