 Men who have high amounts of fat in their abdomens and thighs may have greater risk of developing advanced and fatal prostate cancer than those with less fat in those areas, according to a new study led by researchers from Harvard T.H. Chan School of Public Health.
Men who have high amounts of fat in their abdomens and thighs may have greater risk of developing advanced and fatal prostate cancer than those with less fat in those areas, according to a new study led by researchers from Harvard T.H. Chan School of Public Health.
The association was stronger among men with a lower body mass index (BMI) than with a higher BMI, first author Barbra Dickerman, a research fellow in the Department of Epidemiology, said in a news release.
Diet and exercise to lose fat may decrease the risk of developing prostate cancer, the researchers said.
This was a prospective study of 1832 men in the Age, Gene/Environment Susceptibility–Reykjavik study.
From 2002 to 2006, participants underwent baseline computed tomography imaging of fat deposition, bioelectric impedance analysis, and measurement of body mass index (BMI) and waist circumference.
Men were followed through linkage with nationwide cancer registries for the incidence of total, high-grade, advanced, and fatal prostate cancer through 2015.
Cox regression was used to evaluate the association between adiposity measures and prostate cancer outcomes.
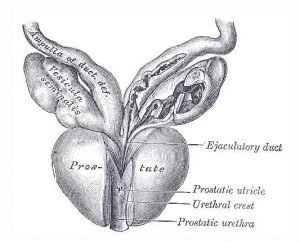
Prostate Gray’s Anatomy
Among the group, 172 men developed prostate cancer, leading to 31 deaths.
Among all men, visceral fat and thigh subcutaneous fat were associated with risk of advanced and fatal disease, respectively.
Among men who were leaner based on BMI, visceral fat was associated with both advanced and fatal disease.
BMI and waist circumference were associated with a higher risk of advanced and fatal disease.
No adiposity measures were associated with total or high-grade disease.
See also:
Normal weight and wider waist in older persons tied to higher dementia risk (2019-12-10)
Link…
Men with Belly Fat at Risk for Osteoporosis (2012/12/17)
Link…
Health-related quality of life, belly fat and testosterone levels (2014-01-22)
Link…
A third way to slow the aging process (2014-01-09)
Link…
Belly fat may be worse than obesity (2015-11-11)
Link…
For more information
Cancer
Body fat distribution on computed tomography imaging and prostate cancer risk and mortality in the AGES-Reykjavik study
Link…
Harvard T.H. Chan School of Public Health
Link…
MDN
This post is also available in:
 Italian
Italian