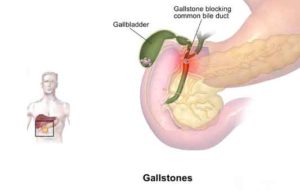
 To treat symptomatic uncomplicated gallstones surgery may not always be necessary: many patients with gallstones and abdominal pain don’t feel better after a cholecystectomy.
To treat symptomatic uncomplicated gallstones surgery may not always be necessary: many patients with gallstones and abdominal pain don’t feel better after a cholecystectomy.
Around 20% of adults in the western world have gallstones, but only one in five patients with gallstones ever develops symptoms.
Because patients with abdominal pain present frequently to general practitioners or to specialist care and often receive a scan, finding gallstones or sludge during work-up has a high a priori likelihood and they are easily attributed as a cause of the symptoms.
International guidelines advise laparoscopic cholecystectomy to treat symptomatic, uncomplicated gallstones.
Despite successful cholecystectomy, some patients might have persisting symptoms (so-called post-cholecystectomy syndrome), a poorly defined state with no clear consensus noted in up to 33% of patients in observational cohorts and randomised trials.
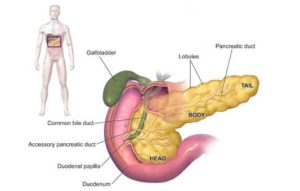
With such a high proportion of patients having symptoms after cholecystectomy, one could intuitively conclude that a more restrictive attitude to surgery would improve outcomes, or be just as effective.
Suboptimal pain reduction in patients with gallstones and abdominal pain was noted with both usual care and following a restrictive strategy for selection for cholecystectomy.
However, the restrictive strategy was associated with fewer cholecystectomies.
The findings should encourage physicians involved in the care of patients with gallstones to rethink cholecystectomy, and to be more careful in advising a surgical approach in patients with gallstones and abdominal symptoms.
For more information
Pain after cholecystectomy for symptomatic gallstones
Link…
Restrictive strategy versus usual care for cholecystectomy in patients with gallstones and abdominal pain (SECURE): a multicentre, randomised, parallel-arm, non-inferiority trial
Link…
MDN
This post is also available in:
 Italian
Italian