|
Scientists have identified a pathway that leads to
the formation of atypical blood vessels that can
cause blindness in people with age-related macular
degeneration.
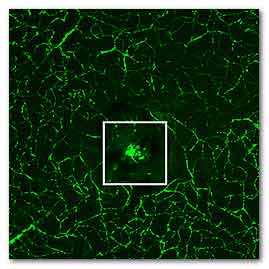
In this image of the retina, normal blood vessels
(green) surround a clump of new, abnormal vessels
that has formed beneath the center of the retina.
Scientists at Washington University School of
Medicine in St. Louis have identified a molecular
pathway that leads to the formation of such blood
vessels, which can cause blindness in people with
age-related macular degeneration.
The research, at Washington University School of
Medicine in St. Louis, sheds light on one of the
leading causes of blindness in industrialized
countries and offers potential targets for treating
the disease.
The study is published online Aug. 11 in the journal
Nature Communications.
“Our research increases our understanding of how
specific immune cells can contribute to vision loss
in macular degeneration, and it also may help us
identify treatments by giving us a molecular pathway
to target,” said principal investigator and retina
specialist Rajendra S. Apte, MD, PhD. “When we
inhibit this pathway, we can alter the immune cells
and interfere with abnormal blood vessel growth in
mice. Doing so might open therapeutic avenues to
halt vision loss or even restore sight in people who
have macular degeneration, the leading cause of
blindness in people over 50.”
Apte, the Paul Cibis Distinguished Professor of
Ophthalmology and Visual Sciences at the School of
Medicine, has spent years studying the immune system
in the eye to distinguish changes related to aging
from those related to disease. In earlier work, he
found that a cell-signaling molecule, called
interleukin-10 (IL10), plays a role in the formation
of blood vessels involved in the “wet” form of
macular degeneration, which is more frequently
linked to blindness than the “dry” form of the
disease.
Before vision loss occurs, IL10 levels increase in
the eye, as do the number of specific immune cells,
called M2 macrophages. These macrophages are known
to contribute to the development of damaging blood
vessel growth beneath the retina.
Until now, though, how IL10 actually contributed to
the proliferation of macrophages and damaging blood
vessels wasn’t well understood.
So Apte and his colleagues engineered mice in which
various cell-signaling pathways were disabled. Those
experiments led them to discover that a specific
signaling pathway involving a protein called STAT3
was activating and altering immune cells in the eye,
and those cells then spurred the formation of
harmful blood vessels.
Further, they examined eye tissue from patients
treated in the 1980s and 1990s, when surgery to
remove abnormal blood vessels from underneath the
retina was routinely performed on patients with the
wet form of macular degeneration. There, too, the
same STAT3 protein that was abundant and active in
M2 macrophages in mice also was found in high levels
in the human tissue.
The findings suggest that the causes of damaging
blood vessel growth in people are the same as what
the researchers had observed in mouse models, Apte
said. In both mice and in patients, abnormal blood
vessel growth was linked to macrophages with high
levels of the active form of STAT3.
That a cause of significant vision loss appears to
be the same in mice and people is good news, Apte
explained, because some compounds can disrupt the
actions of STAT3 in mice and keep the pathway from
spurring blood vessel growth. Those same compounds
may alter the course of macular degeneration in
people with the condition.
“Now that we have a better idea of how these
macrophages are activated at the molecular level, we
may be able to use those drugs to halt or reverse
the disease process,” Apte said.
For more information
Nature Communications
Nakamura R, Sene A, Santeford A, Gdoura A, Kubota S,
Azpata N, Apte RS.
IL10 driven STAT3 signaling in senescent macrophages
promotes pathological eye angiogenesis.
Link...
Washington University School of Medicine in St.
Louis
Link...
MDN |