|
Scientists have repaired a damaged liver in a mouse
by transplanting stem cells grown in the laboratory.
It is the first time researchers have restored
function to a severely damaged liver in a living
animal using stem cells.
It’s just one example of scientists growing tiny
versions of organs in animals and in the lab to
study development and disease, and test potential
treatments. Many of these organs also represent the
first steps towards growing whole organs – or parts
of organs – for transplant.
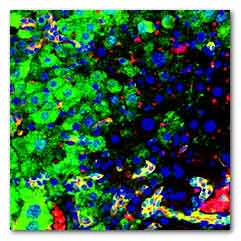
IMAGE - Transplanted hepatic progenitor cells can
self-renew (yellow) and differentiate into
hepatocytes (green) to repair the damaged liver
(Image: Wei-Yu Lu, MRC Centre for Regenerative
Medicine, The University of Edinburgh’)
Researchers from the Medical Research Council (MRC)
Centre for Regenerative Medicine at the University
of Edinburgh transplanted liver stem cells into mice
with liver failure. They found that over several
months major areas of the liver were regrown from
these cells, improving the structure and function of
their livers.
The liver has a great capacity to repair itself,
however in conditions such as cirrhosis and acute
liver failure, it becomes damaged beyond repair.
Within the liver, hepatocytes are the essential
cells that make many proteins and break down toxins,
and while they have been used for transplantation
their use has been limited as they don’t grow well
under laboratory conditions. Liver stem cells
overcome this as they can be grown under laboratory
conditions and have the flexibility to change into
hepatocytes or other important types of liver cells.
This is the first time that researchers have proven
that liver stem cells can regrow the liver to such
an extent. If they can show the same effect with
human cells then they may be useful as a treatment
for liver failure. Transplanting such cells into
patients with liver failure could one-day offer an
alternative to liver transplants.
In the long term, scientists hope to find a way of
stimulating the patient’s own stem cells to repair
the damaged liver using medicines.
The research was funded by the Medical Research
Council, the UK Regenerative Medicine Platformopens
in new window and the Wellcome Trustopens in new
window. It is published in the journal Nature Cell
Biology.
Small organs, or parts of them, are useful for
studying both development and disease, and for
toxicity testing or testing new treatments. In some
cases, mini organs will be able to replace research
using animals.
But they also offer a tantalising glimpse of a world
in which we can grow complex solid organs for
transplant. These tiny organs – often more like
proto-organs with just some of an organ’s functions
– are quite literally ‘starting small’, first seeing
if it’s even possible.
Here we list seven tiny organs that have been grown
so far.
Itty-bitty intestines
In a study at the Cincinnati Children’s Hospital
Medical Center, researchers used induced pluripotent
stem cells to grow human intestinal tissue in the
lab. They then connected the tissue to the kidney of
a mouse, providing it with a blood supply to allow
it to mature into a piece of human intestine. This
technique could provide a useful way of studying and
ultimately treating gastrointestinal diseases in the
future.
Compact kidneys
Working lab-grown kidneys have been transplanted
into rats by researchers from the Center for
Regenerative Medicine in the US. The team stripped
down a rat kidney to a scaffold-like structure,
before introducing rat kidney and blood vessel cells
that grew into a new functioning kidney. They then
transplanted the organ into rats where it
successfully filtered blood and produced urine.
Small skin
An MRC-funded team led by King’s College London and
the San Francisco Veteran Affairs Medical Center has
grown a 3D piece of skin in the lab. Using induced
pluripotent stem cells, they produced an unlimited
supply of skin cells, some of which were then used
to grow a small piece of skin. The lab-grown skin
has a working natural barrier that protects it from
losing moisture, and prevents it from absorbing
chemicals and toxins. This makes it particularly
useful for studying a range of skin conditions, and
for testing drugs and cosmetics.
Tiny thymi
The thymus is an immune system organ which sits just
in front the heart. Another group of researchers at
the MRC Centre for Regenerative Medicine have
reprogrammed mouse cells called fibroblasts, which
normally become connective tissue, to instead become
thymus cells. When mixed with other thymus cell
types and transplanted into mice, the cells grew
into a functioning mouse thymus.
Teeny tickers
Miniature human hearts have been grown in the lab
using a mouse heart ‘scaffold’. Researchers from the
University of Pittsburgh removed all the cells from
a mouse heart, leaving a skeleton-like structure,
before reintroducing immature human heart cells.
After just a few weeks the cells developed into
beating heart tissue.
Small-scale stomachs
Three-dimensional human gastric tissue has been
grown by a team at the Cincinnati Children’s
Hospital Medical Center using human pluripotent stem
cells that were coaxed into becoming stomach cells.
The structures are only three millimetres in
diameter, but could turn out to be useful disease
models for understanding how the stomach develops
and is affected by different diseases. Plans are
already underway to use these tiny organs for
studying how the bacterium, H. pylori, causes
stomach ulcers and gastric disease.
It’s worth mentioning that while we’re talking about
tiny organs, Prof Martin Birchall at University
College London has successfully transplanted stem
cell-based tracheas and larynxes into patients.
link...
For mor information
Liver...
Tiny-organs-grown-by-scientists...
MDN |