|
Research from UW Medicine and collaborators
indicates that a drug-like molecule can activate
innate immunity and induce genes to control
infection in a range of RNA viruses, including West
Nile, dengue, hepatitis C, influenza A, respiratory
syncytial, Nipah, Lassa and Ebola.
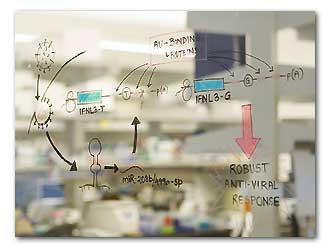
A scientist's illustration of immunology research at
UW Medicine's South Lake Union campus.
The findings, published in the Journal of Virology,
show promising evidence for creating a
broad-spectrum antiviral.
“Our compound has an antiviral effect against all
these viruses,” said Michael Gale Jr., University of
Washington professor of immunology and director of
the UW Center for Innate Immunity and Immune
Disease. The finding emerged from research by his
lab in concert with scientists at Kineta Inc. and
the University of Texas at Galveston.
Gale said he thinks the findings are the first to
show that innate immunity can be triggered
therapeutically through a molecule present in all
our cells, known as RIG-I.
RIG-I is a cellular protein known as a pathogen
recognition receptor. These receptors detect viral
RNA and signal an innate immune response inside the
cell that is essential for limiting and controlling
viral infections. The signal induces the expression
of many innate immune and antiviral genes and the
production of antiviral gene products,
pro-inflammatory cytokines, chemokines and
interferons.
“These products act in concert to suppress and
control virus infection,” the researchers wrote.
Such activation of the innate immune response to
control viral infection has been tested successfully
in cells and in mice. Next steps would be to test
dosing and stability in animal models and then in
humans, a process that could take two to five years,
Gale said.
Currently, there are no known broad-spectrum
antiviral drugs and few therapeutic options against
infection by RNA viruses. RNA viruses pose a
significant public health problem worldwide because
their high mutation rate allows them to escape the
immune response. They are a frequent cause of
emerging and re-emerging viral infections. West Nile
virus infections, for example, started in the United
States in 2000 and remerged in 2012. The World
Health Organization reports 50 million to 100
million new cases of dengue fever yearly and 22,000
deaths caused by the related dengue virus. Dengue is
now present in the southern U.S.
Hepatitis C, which is transmitted through the blood,
infects upward of 4 million people each year; 150
million people are chronically infected and at risk
for developing cirrhosis or liver cancer, according
to the paper. Direct-acting antivirals can control
hepatitis C and show promise of long-term cure, but
viral mutation to drug resistance is a concern with
prolonged use of these drugs. Also the drugs’
exorbitant costs make them unaffordable to many or
most patients.
"There is tremendous interest in triggering innate
immunity," said Shawn Iadonato, chief scientific
officer at Seattle biotech Kineta. Some viral
infections, he pointed out, cannot be treated by
traditional antivirals. Activating innate immunity
also will make the viruses less likely to resist the
drug actions because the therapy targets the cell,
via gene action, rather than the virus itself.
“It’s routine for us to think of broad-spectrum
antibiotics, but the equivalent for virology doesn’t
exist,” Iadonato said.
For more information
Journal of Virology
Targeting innate immunity for antiviral therapy
through small molecule agonists of the RLR pathway
J. Virol. doi:10.1128/JVI.02202-15
Link...
UW Center for Innate Immunity and Immune Disease
Link...
MDN |